How can we help?
888-283-1722
Call us now at 888-283-1722
24/7 Referrals and Nursing Support
Voices of Care Blog
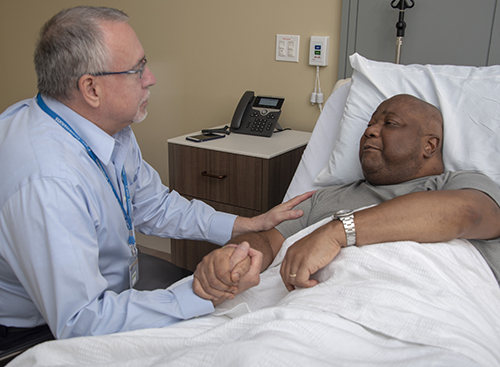
What Every Family Should Know About Medical Treatment at End of Life
Posted on March 30, 2020 by Robert M. Taylor, MD, FAAHPM, FAANPatients referred to hospice typically have reached a point where treatments to slow the progression of their disease are no longer effective or cause intolerable side effects, or both. The focus of treatments in hospice is to control the patient’s symptoms without accelerating the disease process.
Although patients must be terminally ill to qualify for hospice, they usually are not actively dying when they enroll. Their life expectancy is limited - usually to six months, rarely to a year or two - but we don’t know exactly when their death will occur. At some point, however, we usually will have an indication that the person is approaching death. That is the time we consider a person to be “actively dying.” This usually becomes apparent a few days before death.
When caring for an actively dying patient, our goals are:
-
To assure a peaceful and comfortable death for the patient.
-
To assure that the family understands why certain treatments may be stopped and others may be started.
The best way to care for somebody who is terminally ill – but not actively dying – is somewhat different than how you care for a person who is actively dying. Many of the things you would do for the former would be harmful to the latter and, of course, vice versa.
I’d like to address some misconceptions about best courses of treatment for hospice patients at end of life.
Myth #1 – Hydration will help an actively dying patient.
When the person is actively dying, it is important to recognize that their body is shutting down and cannot tolerate many of the things that a healthy person could. For example, the kidneys begin to shut down so they cannot rid their body of excess fluid. Thus, IV fluids, which help many sick people survive a serious illness, are actually harmful and cause discomfort in a dying patient. When excess fluid accumulates in their body, the lungs typically become wet and oxygen cannot penetrate through the lung tissue to the blood stream, so the person will struggle for breath. Lung tissue is a lot like tissue paper – when tissue paper is dry you can blow through it, but when it is wet, you cannot. Thus it is always most comfortable to be a little dehydrated when dying – any sense of thirst can usually be managed by keeping the mouth and lips moist, with swabs or lollipops and lip gloss.
Myth #2 – Medications used to comfort actively dying patients will accelerate the dying process.
Sometimes the use of comfort medications prolongs the dying process as it reduces the stress on the heart by decreasing pain and other distressing symptoms. In fact, sometimes patients will be in distress and appear to be within minutes to hours of dying but, when medications are administered to relieve their symptoms – usually sedating them as well – the stress on their heart and other organs is diminished so they end up living longer than anticipated, but remaining comfortable through those final hours and days.
Myth #3 – Providing food and supplemental oxygen at end of life will improve patients’ comfort.
It is common for family members, and even patients themselves, to assume that weight loss is a result of the patient not eating enough. The reality is usually more complicated, however. Many advanced diseases, including cancer, result in weight loss even when patients eat adequately, because their body cannot properly absorb and utilize nutrition. Exactly why this happens is complex, but one way of thinking about it is that the cancer “steals” the nutrition from the healthy body to nourish the cancer. This is important for several reasons. Most importantly, forcing oneself to eat more will not typically result in weight gain – the problem is not how much food they are putting into their stomach, but rather that the food ingested is being diverted to feed the cancer instead of the healthy body.
Similarly, when patients are awake and feeling short of breath, oxygen can make them feel much better. However, when a patient is dying, and they are no longer awake, the oxygen level in their blood will eventually fall, due to diminished respiratory drive. Thus, supplemental oxygen in that situation prolongs the dying process without improving comfort.
Death is one of the inevitable mysteries of life and almost always causes heartbreak, but when a dying patient is properly cared for, his or her suffering usually can be minimized. I hope this information I’ve offered will help patients and families prepare for, and cope with, treatment changes that will be recommended by the hospice team during the final few days of life.
Learn more about hospice with Care Dimensions.
About the author
Robert Taylor, MD, FAAHPM, FAAN, has been associate medical director at Care Dimensions since 2017 and is retiring in April 2020. Prior to joining Care Dimensions, he was the medical director of the Ohio State University Palliative Care program for 10 years.
Additional Posts
Finding Purpose in Hospice Care: My 45 Years as a Volunteer
Posted on May 16, 2025 by Gail Thompson in Hospice, Kaplan Family Hospice House, VolunteersOver the past four decades, Gail Thompson's connection to hospice has gone from personal loss to profound purpose. She shares the rewards of supporting families through life's most difficult transitions as a hospice volunteer. ...
Continue readingFinding My Niche: Life as a Hospice Nurse
Posted on May 6, 2025 by Patrick Davidson, RN Case Manager in Hospice, Hospice careersFor nurse Patrick Davidson, there's something profoundly meaningful about working in hospice. He discusses the challenges and the rewards of the profession. ...
Continue readingFor Hospice Nurse, It’s All About Teamwork
Posted on May 5, 2025 by Debbye Lindberg, RN Case Manager in Hospice, Hospice careersFor nurse Debbye Lindberg, hospice is all about teamwork. She talks about how a team approach ensures patients and families get the best care possible. ...
Continue readingAnyone—patient, family, care provider—can make a referral. Fill in the form online or call us today.
Since 1978, Care Dimensions, formerly Hospice of the North Shore, has provided comprehensive and compassionate care for individuals and families dealing with life-threatening illnesses. As the non-profit leader in advanced illness care, we offer services in over 100 communities in Massachusetts.
Copyright 2025 | Care Dimensions, 75 Sylvan Street, Suite B-102, Danvers, MA 01923 | 888-283-1722 | 978-774-7566 |